For years, millions of women have known the condition as PCOS or PCOD — terms often associated with irregular periods, hormonal imbalance, acne, weight gain and fertility concerns. Now, there has been a major shift in how the condition is understood and described.
PCOS, or Polycystic Ovary Syndrome, is now renamed as PMOS: Polyendocrine Metabolic Ovarian Syndrome. The change aims to reflect what doctors and researchers have increasingly recognised over the years — that the condition is not just about ovarian cysts, but a complex whole-body hormonal and metabolic disorder.
To understand what this change means for patients, diagnosis and long-term care, we spoke to Dr Yash Bahuguna, MBBS, MS, DNB, a gynaecologist at Pinky Promise.
With over six years of clinical experience across institutions, he specialises in hormonal health and PCOS/PMOS care.
Excerpts from the interview:
1. There has been a shift from PCOD/PCOS to PMOS. What exactly has changed, and why?
The condition earlier called PCOS is now being renamed PMOS.
The change is important because the older name over-focused on “cysts” and ovaries, while the condition is actually a broader hormonal, metabolic and reproductive health disorder.
PMOS affects weight, metabolism, mental health, skin and reproductive health. The older name also contributed to missed diagnoses and inadequate treatment in many cases.
2. What do PCOD, PCOS and PMOS mean? Are PCOS and PCOD invalid now?
PCOD usually stands for Polycystic Ovarian Disease. It is an older, commonly used term in India, but medically, PCOS has been the more accepted term.
PCOS stands for Polycystic Ovary Syndrome. This has been the standard medical term for decades.
PMOS stands for Polyendocrine Metabolic Ovarian Syndrome. This is the newer term proposed to better describe the condition.
PCOS and PCOD are not becoming “invalid” overnight. Patients, doctors, hospitals and insurance systems will continue using them during the transition. However, medically, PMOS is considered more accurate because it reflects the condition’s whole-body impact.
3. Is PMOS now medically accepted globally?
PMOS has been announced through a major global effort led by Monash University and published in The Lancet.
The process reportedly involved 14 years of work, more than 22,000 survey responses, and 56 patient and professional organisations.
Full implementation is expected through a three-year transition, with the updated international guideline expected in 2028.
So yes, this marks a significant international shift, though adoption across doctors, countries, coding systems and insurance systems will take time.
4. Why is the older terminology inaccurate?
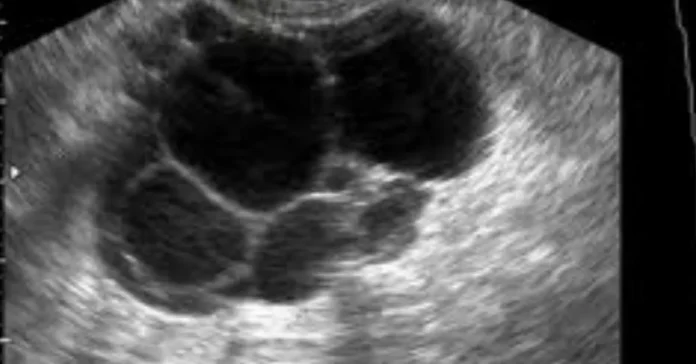
Most people with this condition do not actually have ovarian cysts.
What is often seen on ultrasound are small, immature follicles, not abnormal cysts. In addition, some patients may not have classic irregular periods or other “typical” symptoms.
The older terminology made the condition appear ovarian-specific, when in reality it is driven by complex endocrine and metabolic dysfunction.
/filters:format(webp)/english-betterindia/media/media_files/2026/05/14/117724-2026-05-14-12-25-45.jpg)
5. Does the name change alter diagnosis or treatment?
Not immediately.
The name has changed, but diagnosis and treatment still follow established clinical guidelines. The 2023 international guideline continues to use features such as ovulatory dysfunction, clinical or biochemical hyperandrogenism, and ovarian morphology or AMH levels where appropriate.
Treatment also remains personalised. This may include lifestyle changes, menstrual regulation, acne and hair-growth management, insulin-resistance management, fertility support where needed, and long-term metabolic risk reduction.
6. Why does this name change matter medically?
Names shape how doctors think.
If the name says ‘cysts,’ care becomes ultrasound-focused. If the name says ‘metabolic’ and ‘endocrine,’ doctors are more likely to screen for insulin resistance, weight changes, diabetes risk, mental health concerns and long-term cardiovascular risk.
/filters:format(webp)/english-betterindia/media/media_files/2026/05/14/2-2026-05-14-12-26-42.jpg)
So this is not merely cosmetic. It can change clinical behaviour.
7. How can someone know they may have PMOS?
PMOS may show up as:
-
Irregular or delayed periods
-
Acne
-
Excess facial or body hair
-
Weight gain or difficulty losing weight
-
Darkened skin folds
-
Sugar cravings or fatigue
-
Mood changes, anxiety or depression
/filters:format(webp)/english-betterindia/media/media_files/2026/05/14/1-2026-05-14-12-26-57.jpg)
Not every patient experiences every symptom, which is why clinical evaluation is important.
8. What are the biggest myths around PCOD/PMOS?
According to Dr Bahuguna, some of the biggest myths are:
-
“Everyone with PCOS has cysts.” — Not true.
-
“You must be overweight to have it.” — Not true. Lean patients can also have it.
-
“It only affects fertility.” — Not true. It affects metabolic and long-term health too.
-
“Birth control pills cure it.” — They may control symptoms, but they do not cure the underlying tendency.
-
“You cannot get pregnant with PCOS/PMOS.” — Many women conceive naturally or with treatment.
9. What are the earliest signs teenagers and young adults should watch for?
Some early signs include:
-
Irregular periods for more than two to three years post menarche or missing your period for more than 3 months without pregnancy.
-
Severe acne not responding to routine care
-
Excess facial hair
-
Sudden weight gain
-
Dark pigmentation around the neck or underarms
-
Hair thinning
-
Mood swings linked to cycle issues
-
Strong family history of PCOS, diabetes or metabolic disease
However, teenagers should avoid self-diagnosis. Careful medical assessment is important because normal puberty can sometimes mimic PMOS symptoms.
10. Is PMOS mainly caused by lifestyle, or is it genetic and hormonal?
PMOS is not simply a “lifestyle disease”.
It has strong hormonal, metabolic and genetic influences. Lifestyle factors can worsen or improve symptoms, but they are not the sole cause.
/filters:format(webp)/english-betterindia/media/media_files/2026/05/14/4-2026-05-14-12-27-12.jpg)
Many patients have insulin resistance, androgen excess or a family history of metabolic conditions. Food, sleep, stress, physical activity and weight changes may influence severity, but they do not fully explain the condition.
11. What are the long-term risks if PMOS is ignored?
Untreated PMOS may increase the risk of:
-
Type 2 diabetes
-
Heart disease
-
High cholesterol
-
Fatty liver disease
-
High blood pressure
-
Infertility or ovulation problems
-
Endometrial hyperplasia in those with long gaps between periods
-
Anxiety, depression and body-image distress
-
Pregnancy complications
“This is why long-term care matters, not just period regulation,” Dr Bahuguna explains.
12. What genuinely helps in managing PMOS?
According to Dr Bahuguna, the most effective approach is comprehensive and personalised care, including:
-
Balanced, protein- and fibre-rich meals
-
Regular strength training and movement
-
Good sleep and stress management
-
Weight management where relevant
-
Screening for insulin resistance, lipid levels and diabetes risk
-
Medical treatment for irregular cycles, acne, excess hair growth or fertility concerns
-
Metformin or other insulin-sensitising support where clinically indicated
-
Mental health support
-
Long-term follow-up instead of one-time prescriptions
“The key message is that PMOS is manageable, but it requires whole-body care,” he says.
The bigger shift behind the new name
The move from PCOS to PMOS is more than a terminology update. It reflects a broader understanding of a condition that affects far more than reproductive health alone.
By shifting focus from “cysts” to metabolism, hormones and long-term health, experts hope the new terminology will encourage earlier diagnosis, more comprehensive treatment and greater awareness about the condition’s impact on both physical and mental well-being.
For patients, the message is reassuring: while the name may be changing, the goal remains the same — better understanding, better care and better long-term health outcomes.
Disclaimer : This story is auto aggregated by a computer programme and has not been created or edited by DOWNTHENEWS. Publisher: thebetterindia.com